
Latest News


Schizophrenia care starts with seeing the whole person
For the first time in a decade, a new set of clinical guidelines for schizophrenia care in Australia and Aotearoa New Zealand has been published to reflect new evidence and approaches to treatment.
People living with schizophrenia face significantly shorter life expectancies than the general population, often due to their physical health needs. To address this, QCMHR Research Affiliate Professor Shuichi Suetani led the development of new guidelines that emphasise care treating the whole person, not just the diagnosis.
"Guidelines influence real decisions in real lives," Professor Suetani says. "As evidence evolves, updated guidance can help people receive care that is more informed and better aligned with their needs.”
“To develop these new guidelines, we used the GRADE approach, which looks at both what the research shows and the strength and reliability of the research. In practice, it means the guidelines reflect not only what has been found, but also how confident we can be when making recommendations for care.”
"Schizophrenia affects every part of a person's life, their physical health, their relationships, their ability to work and connect with their community. The new guidelines aim to reflect that reality,” Professor Suetani says.
The updated guidelines organise schizophrenia care into seven key areas:
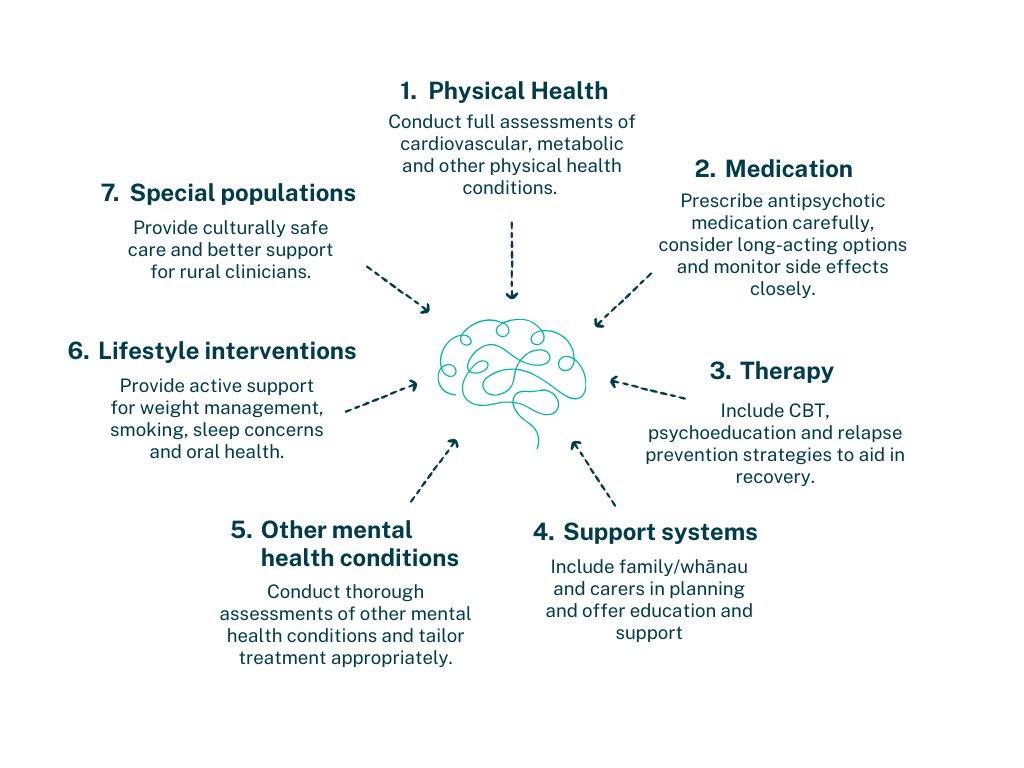
Physical health: A comprehensive physical health assessment from the very start of treatment is essential with continued, regular monitoring. Physical health needs are too often missed or not prioritised and the guidelines are clear that this needs to change.
Medication: Antipsychotic medication remains central to treatment, but the guidelines recommend starting with options that are gentler on physical health and tailored to the individual. Long-acting injectable medications are highlighted as a strong option for long-term stability, and clozapine remains essential for those with treatment-resistant schizophrenia.
Therapy: Psychosocial therapies should be considered from the very start of treatment and throughout. Cognitive Behavioural Therapy for psychosis, psychoeducation and relapse-prevention strategies can all help with symptom management and recovery.
Family/whānau and carer involvement: Strong support systems are crucial to long-term recovery. Schizophrenia doesn’t just affect one person. When support systems are informed and included, people feel less alone and outcomes improve for everyone.
Psychiatric comorbidities: People living with schizophrenia commonly experience other mental health conditions alongside their diagnosis. These conditions require thorough assessment and tailored treatment, acknowledging that symptoms can be easily overlooked or mistaken for schizophrenia itself.
Lifestyle interventions: Physical activity has some of the strongest evidence for improving mental health symptoms in schizophrenia, particularly negative symptoms which often respond poorly to medication alone. The guidelines recommend structured exercise programmes and active support for weight management, smoking, sleep and oral health.
Special populations: Māori and Aboriginal and Torres Strait Islander peoples face higher rates of schizophrenia and greater barriers to culturally safe care. People in rural and regional areas are also highlighted, where access to psychiatrists is limited and GPs often carry the primary responsibility for care. The guidelines call for culturally safe practice and better support for rural clinicians.
The overall approach of the new guidelines emphasises quality of life and autonomy, not just symptom reduction. This means collaborative treatment decisions, personalised care plans and supporting people to live long, healthy and fulfilling lives.
“A lot has changed since the last major guidelines were released in 2016 and it’s important that guidance is revisited as new evidence comes to light,” Professor Suetani says.
For clinicians, that updated evidence brings greater clarity and confidence in the decisions they make every day. For the thousands of people living with schizophrenia and those who support them it means care that is more consistent, more transparent and more grounded in what works.
Schizophrenia care works best when it sees the whole person and these guidelines are a meaningful step toward making that the standard, not the exception.
Established in 1987, QCMHR is funded by Queensland Health to work state-wide and contribute to the local, national, and global research efforts to improve mental health.
New guidelines for management of schizophrenia in Australia and Aotearoa New Zealand
Media contact:
Laura Corcoran, Research Communications Officer

HEAD OFFICE
Level 3, Dawson House
The Park Centre for Mental Health Treatment
Research and Education, Wacol, QLD 4076
P: +61 7 3271 8660
ACKNOWLEDGEMENT OF COUNTRY
In the spirit of reconciliation, the Queensland Centre for Mental Health Research (QCMHR) acknowledges the Traditional Owners of the lands in which QCMHR operates and their continuing connections to land, waters and community. We pay our respects to Elders past and present and stand together with all Aboriginal and Torres Strait Islander peoples.
